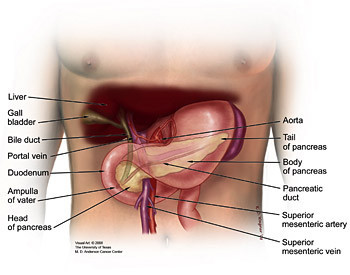
Surgical Treatment Options
Surgery to remove a tumor offers the best chance for long term control of all types of pancreatic cancer. If a tumor is able to be surgically removed, it is called resectable. About 15-20% of patients with pancreatic adenocarcinoma have tumors which are considered surgically resectable.
When is surgery used?
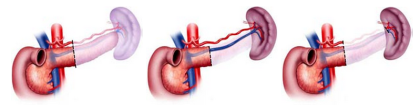
In general, a pancreatic tumor is considered resectable if it has not spread beyond the pancreas and does not involve major arteries. If veins are involved, a qualified surgeon may be able to
perform a vein resection. A vein resection typically adds an extra 60-90 minutes to the length of the surgery.
Determining a patient’s eligibility for surgery is not always easy. Even sophisticated imaging tests may not provide a perfect picture of the tumor. In some cases, during surgery, the surgeon will
find that the cancer has spread and the operation will be ended. If surgery to remove the tumor is not possible, palliative procedures may be considered.
What are the different types of pancreatic surgeries?
Different types of surgery are performed depending on the location of the tumor within the pancreas, there are
also pallative surgies used in treating Pancreatic Cancer.
Whipple Procedure
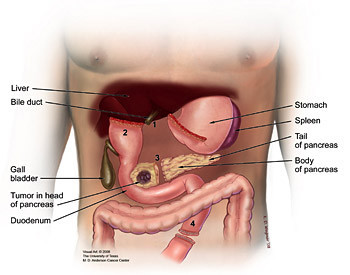
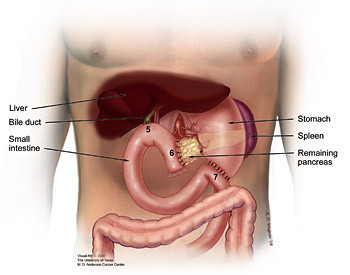
The Whipple Procedure, or pancreaticoduodenectomy, is the most commonly performed surgery to remove tumors in the pancreas. In a standard Whipple procedure, the surgeon removes the head of the pancreas, the gallbladder, part of the duodenum which is the uppermost portion of the small intestine, a small portion of the stomach called the pylorus, and the lymph nodes near the head of the pancreas. The surgeon then reconnects the remaining pancreas and digestive organs so that pancreatic digestive enzymes, bile, and stomach contents will flow into the small intestine during digestion. In another type of Whipple procedure known as pylorus preserving Whipple, the bottom portion of the stomach, or pylorus, is not removed. In both cases, the surgery usually lasts between 6-10 hours.
After a Whipple procedure, the most common complication is delayed gastric emptying, a condition in which the stomach takes too long to empty its contents. Usually, after 7-10 days the stomach begins to work properly. If delayed gastric emptying persists, supplemental feedings by a feeding tube may be started. The condition usually lasts for another 7-10 days, but could last as long as a few weeks. The most serious potential complication is abdominal infection due to leakage where the pancreas has been connected to the intestine. This occurs in approximately 10% of patients and is usually managed by a combination of draining tubes, antibiotics, and supplemental tube feedings. Patients who have undergone the Whipple procedure may experience long-term effects including digestive difficulties.
Distal Pancreatectomy
A distal pancreatectomy is performed if a tumor is located within the body or tail portion of the pancreas. The surgeon removes the body and tail of the pancreas and sometimes the spleen. All other organs are left in place.
The most common complication from a distal pancreatectomy is leakage of pancreatic juices. Other serious complications include bleeding and infection.
Total Pancreatectomy
A total pancreatectomy is performed in the rare situation that the tumor has invaded the head, neck, and tail of the pancreas. Similar to a Whipple procedure, the gallbladder, part of the duodenum which is the uppermost part of the small intestine, bottom portion of the stomach called the pylorus, and local lymph nodes are removed along with the entire pancreas. The spleen may also be removed.
Because the entire pancreas is removed in a total pancreatectomy, the person will be diabetic after surgery and must use insulin to control blood sugar level. The patient will also need to take pancreatic enzyme supplements with meals in order to properly digest food.